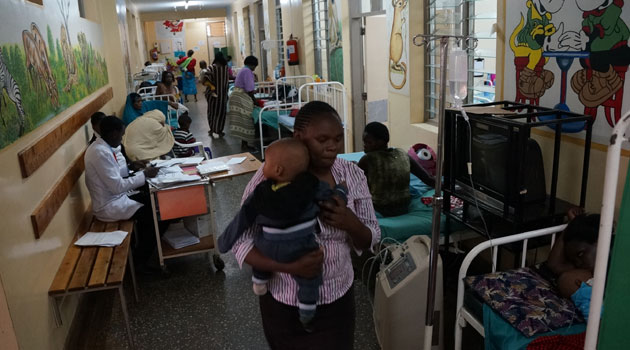
Upon entry into St Mary’s Hospital in Lang’ata, one need not to be told all is in disarray in the health sector/MUTHONI NJUKI
NAIROBI, Kenya, Mar 10 – The grim reality of the doctors’ strike across the country is the chaotic, heart wrenching and obvious suffering of patients who with no other option, troop to the few faith-based hospitals to seek treatment.
Upon entry into St Mary’s Hospital in Lang’ata, one need not to be told all is in disarray in the health sector.
The critically ill lie on the grass outside, others squeeze on few available benches while the stronger ones stand in winding queues waiting for their turn to see the doctor, which can be more than five hours.
Some of the scenes are horrific as most of the patients show up only when diseases have taken a toll on them.
Exhausted but determined to save the life of his wife and two month-old baby, Daniel Osieko fights hard to hold back his tears as he narrates the tormenting moments.

Exhausted but determined to save the life of his wife and two month-old baby, Daniel Osieko fights hard to hold back his tears as he narrates the tormenting moments/MUTHONI NJUKI
His tribulations are deep as words flow endlessly to the point of making those nearby cry.
“My baby came many weeks after the due date. The birth coincided with the doctors’ strike, the baby was unwell and my wife was also unwell. We went to a nearby hospital in Kitengela and we were admitted but we didn’t have enough money so we had to leave,” Osieko narrated as he held his tiny daughter in his arms.
His friends helped him raise some money to support him to come to St Mary’s Hospital in Nairobi. Though the condition of his baby and wife is under control, some Sh300,000 is still required for full treatment which he says he doesn’t have.
His hope is that services can resume at public hospitals since he has his NHIF card that can cater for treatment.
Every patient we met at St Mary’s Hospital had a similar story – that of an agonising desperate journey seeking treatment without money and the lengthy period they have to wait before being attended to.
With such large crowds of patients and with most of them presenting late cases of diseases, the ripple effect is a strain on manpower, the resources, equipment and space at hospitals such as St Mary’s.
But most agonising are the high numbers of deaths recorded since the doctors’ strike began 97 days ago.
Capital FM News spoke to Dr Kimani Ngaruiya, Consultant Paediatrician and Clinical Director at the hospital.
From the usual 800 -1,000 patients a day the hospital used to receive prior to the strike, the numbers have now tripled.
“At the onset of the strike, that number continued to increase steadily. By end of December we were seeing three times that number to date,” he explained.
As we walked from ward to ward, the reality of the doctors’ strike left us distressed.
Every smallest available space was utilised to accommodate extra beds, be it along the corridors or walking spaces between the beds.
“We cannot turn away patients, we have created every space we could to accommodate the high number of patients,” Dr Kimani explained as he guided us through the crowded wards and corridors at the hospital.
The maternity ward which has a bed capacity of 40 now has 100 patients.
The hospital used to deliver about 30 mothers a day and today it is talking of 60 deliveries daily.
“There are challenges of these mothers being delivered when it is too late and coming from far flung areas. We have had very bad cases of complications of mothers laboured beyond what is recommended having laboured for over 18 hours. Some have come with ruptured uteruses,” he regretted.
The unprecedented high patient turnout, Dr Ngaruiya explained overwhelmed the hospital’s space, equipment and other supplies.
The disturbing state of affairs has not spared the hospital staff from the burnout of working longer hours without leave.
“We decided to be able to cope up with this, then we had to tell our staff to more work extra and did not sign their leaves as some had scheduled,” he said.
Due to the late presentation of cases at the hospital, the number of deaths since the doctors’ strike began last December had increased to shocking numbers.
“Of course with the increased number it is usually implies that there will be a proportionate increase in the number of deaths despite the best efforts.”
In the paediatric department for example, the annual infant mortality rate at the hospital was below 1.5 per cent and following the doctors’ strike the number had shot up to a death rate of over 5 per cent according to Dr Ngaruiya.
Contributing factors, he explained stemmed from prolonged labour and birth complications which contributed to the high number of pre-term babies yet with a limited number of incubators, surgical wards, Intensive Care Units and other requirements for saving lives.
“Some of the mothers only when they realise their conditions are not improving is when they come to hospital while others had decided to give birth at home until they develop complications,” he stated.
Through his own experience Dr Ngaruiya only hopes that the government could have acted fast and early enough to save lives, reduce pain and suffering of patients he meets on daily basis.
“A strike affecting healthcare is not a strike you would want to prolong even a week because it is about people’s lives. It only requires the goodwill of both parties in terms of negotiations and we would have averted many deaths and they (deaths) will continue to happen as long as there is no solution at hand,” he stated as he supported fellow doctors in their cry for better working terms and conditions in public hospitals.