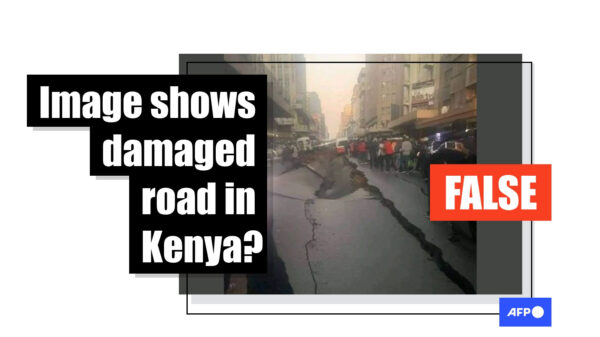
But in a 2008-11 study of PrEP for HIV prevention among African Women (FEM-PrEP) the calculation of risk presented a problem/FILE
It’s lucky then, I tell myself, that I didn’t stare at the couple that sat along the corridor as we made our way into the conference room of the Partners PrEP study facility in Thika.
PrEP, if you’re not familiar, stands for pre-exposure prophylaxis; in layman terms, the prescription of anti-retroviral drugs to persons at high risk of contracting the Human Immunodeficiency Virus (HIV).
It’s worth noting that PrEP differs from PEP, post-exposure prophylaxis given in emergency situations such as rape or when struck by a needle used to draw blood from a person who may be HIV infected.
In the case of the Thika study, the high risk population targeted are those in serodiscordant partnerships – where one partner is HIV negative and the other positive but not yet on anti-retroviral therapy despite a heavy viral load.
“When the couples join the study we put both partners on ARVs for six months, a bridge period, so the seronegative partner is not put at risk while we suppress the virus in the seropositive partner,” Dr Elizabeth Irungu, a research clinician, explains.
The efficacy of PrEP in guarding against the seronegative partner acquiring HIV is not in question with the Thika team having being involved in a study of 4,747 couples for 36 months – beginning July 2008 – that showed Truvada (an anti-retroviral drug) when taken by the seronegative partner was 75 percent efficacious in preventing HIV infection.
“It goes up to 90 percent when adherence is high,” Dr Patrick Ndase, a Research Associate, Department of Health, University of Washington and Regional Physician for the Partners PrEp study says.
The Thika team is now involved in a demonstration project, concluding in 2015, to evaluate, “factors influencing adherence to ART and PrEP, and the decision processes couples follow in making HIV-1 prevention choices,” their study description reads; adherence to antiretroviral therapy (ART) by the seropositive partner and PrEP by the seronegative partner being critical to the prevention of HIV transmission.
“One of the ways we track adherence is by monitoring how often and when the seronegative partners twist open their bottles of Truvada through a monitor in the cap,” Ngure explains.
PrEP has been hailed as the closest thing to a vaccine against HIV and Dr Nase agrees with the late AIDS researcher Jeop Lange, who went down with the infamous Malaysian Airlines flight MHI7and is quoted as having said: “In the end, it may be a lot easier to eradicate HIV through prevention than in the hope for finding a cure.”
READ: Top AIDS official says six colleagues on Malaysia plane, not 100
Beyond preventing seroconversion, becoming HIV positive, PrEP allows serodiscordant couples to conceive without going through the costly procedures of sperm washing and artificial insemination that are out of reach for many.