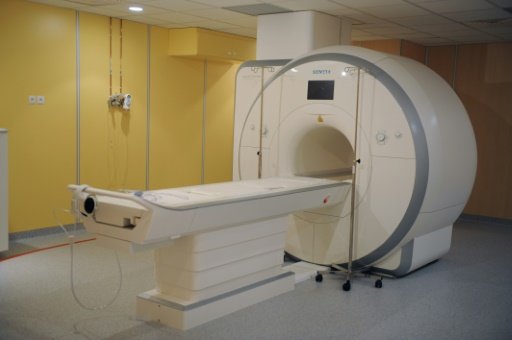
A quarter of men suspected of having prostate cancer could avoid invasive and potentially dangerous biopsies with the help of MRI scans, researchers reported Friday.
Magnetic resonance imaging (MRI) could also reduce the number of men over-diagnosed with the disease by five percent, they detailed in a study published in The Lancet.
The new approach is potentially a game-changer, experts commenting on the study said.
In the case of prostate cancer, “over-diagnosed” includes relatively benign cancers that do not cause any harm during a man’s lifetime.
“Prostate cancer has aggressive and harmless forms,” noted lead author Hashim Ahmed, a surgeon at University College London’s faculty of medicine.
Typically, men undergo a prostate biopsy if they experience certain symptoms or show high levels of a protein in their blood, as detected by a prostate specific antigen (PSA) test.
Each year, over a million prostate biopsies are done in Europe alone.
The procedure — which can cause bleeding, pain and serious infections — involves using a biopsy needle to draw a tissue sample through a small cut made between the anus and scrotum.
The needle goes in “blind,” and can thus bypass a cancerous mass.
“Our current biopsy test can be inaccurate because the tissue samples are taken at random,” Ahmed said in a statement. “It can miss aggressive cancers that are actually there.”
And if the biopsy does finds cancer cells, it cannot reliably determine whether they are malignant.
As a result, some men are given a false diagnosis and prescribed treatments with nasty side effects.
Ahmed and his team wanted to find out if a MRI scan could be used as a “triage” test to determine which men with elevated protein counts might safely avoid a biopsy.
A multi-parametric MRI (MP-MRI) can provide information about a cancer’s size, density, and proximity to the bloodstream.
– Second trial under way –
All of these elements help distinguish between aggressive and benign forms of the disease.
In the study, 576 men spread across 11 public hospitals in Britain and suspected of having prostate cancer were given a MP-MRI scan, followed by two types of biopsy.
One was the type commonly used to detect cancer, and the other was designed to compare the standard biopsy’s accuracy in detecting malignancy against the MRI scans.
Forty percent of the men turned out to have had aggressive cancer.
The scan correctly diagnosed almost all of them (93 percent), whereas the standard biopsy identified only half.
“Our results show that MP-MRI should be used before biopsy” to identify men who have harmless cancers and do not need a biopsy immediately, Ahmed said.
This group however should continue to be monitored by their doctors.
Only those whose scan results point to an aggressive cancer should have a biopsy, to confirm.
Using the two tests in this fashion “could reduce over-diagnosis of harmless cancers by five percent… and improve the detection of aggressive cancers from 48 to 93 percent,” Ahmed concluded.
Reaction from other experts was positive.
“This has the potential to change clinical practice,” said Arnauld Villers, head of the urology department at the Regional University Hospital in Lille, France.
“These results represent a solid basis for a new pathway of diagnosis for prostate cancer detection, leading to fewer biopsies.”
A second clinical trial overseen by Cancer Research UK, currently recruiting volunteers, will seek to validate the study results.
